“It feels like I’m sitting on a nail”
Introduction
Have you ever felt as if you were sitting on a nail? For many people with coccygodynia, the problem begins exactly this way: sitting first feels uncomfortable, then a deep, localized pain gradually appears at the very bottom of the spine. When they stand up, the sensation may become sharp and sudden, as if the area had been compressed for too long.
Coccygodynia is often described as a very specific form of tailbone pain when sitting. Yet despite its distinctive character, it is frequently misunderstood. It may be confused with low back pain, sciatica, or even perineal discomfort, which can delay appropriate interpretation.
In this article, we explore why the coccyx can become such a sensitive focal point, how sitting mechanics can progressively overload it, and why the key distinction is often not simply “injury or no injury,” but structural versus functional. To place this issue within a broader framework, you can also explore our overview of sitting-related pain.
How to Read This Article
- ✔ Purpose: Explain the biomechanical and functional mechanisms involved in coccygodynia.
- ✔ Goal: Help you understand why tailbone pain often worsens in sitting.
- ✔ Use: Clarify how coccyx pain may be local, referred, structural, or functional.
- ✖ Limitation: This article does not replace medical diagnosis or clinical care.
1. The Coccyx: A Small Bone with a Major Mechanical Role
The coccyx is often perceived as an insignificant anatomical remnant. In reality, it plays an important mechanical role. Located at the very bottom of the spine, it is made of three to five fused vertebral segments and serves as an anchoring point for part of the pelvic floor.
It contributes to pelvic balance, supports load transfer at the lower end of the spine, and participates in the relationship between the pelvis and the sitting surface. In practical terms, the coccyx often absorbs what the rest of the body can no longer redistribute efficiently.
As long as this load distribution remains harmonious, the coccyx stays silent. But when imbalance appears, it can become the focal point where mechanical stress accumulates.
2. Limited Mobility: Small Range, Big Consequences
Contrary to popular belief, the coccyx is not a fixed bone. It has a limited but essential physiological mobility, especially during sitting, bowel movements, and childbirth.
This mobility allows the pelvis to adapt to constraints instead of concentrating pressure on a single point. Problems arise when this mobility becomes excessive, restricted, or poorly coordinated with the rest of the pelvic system.
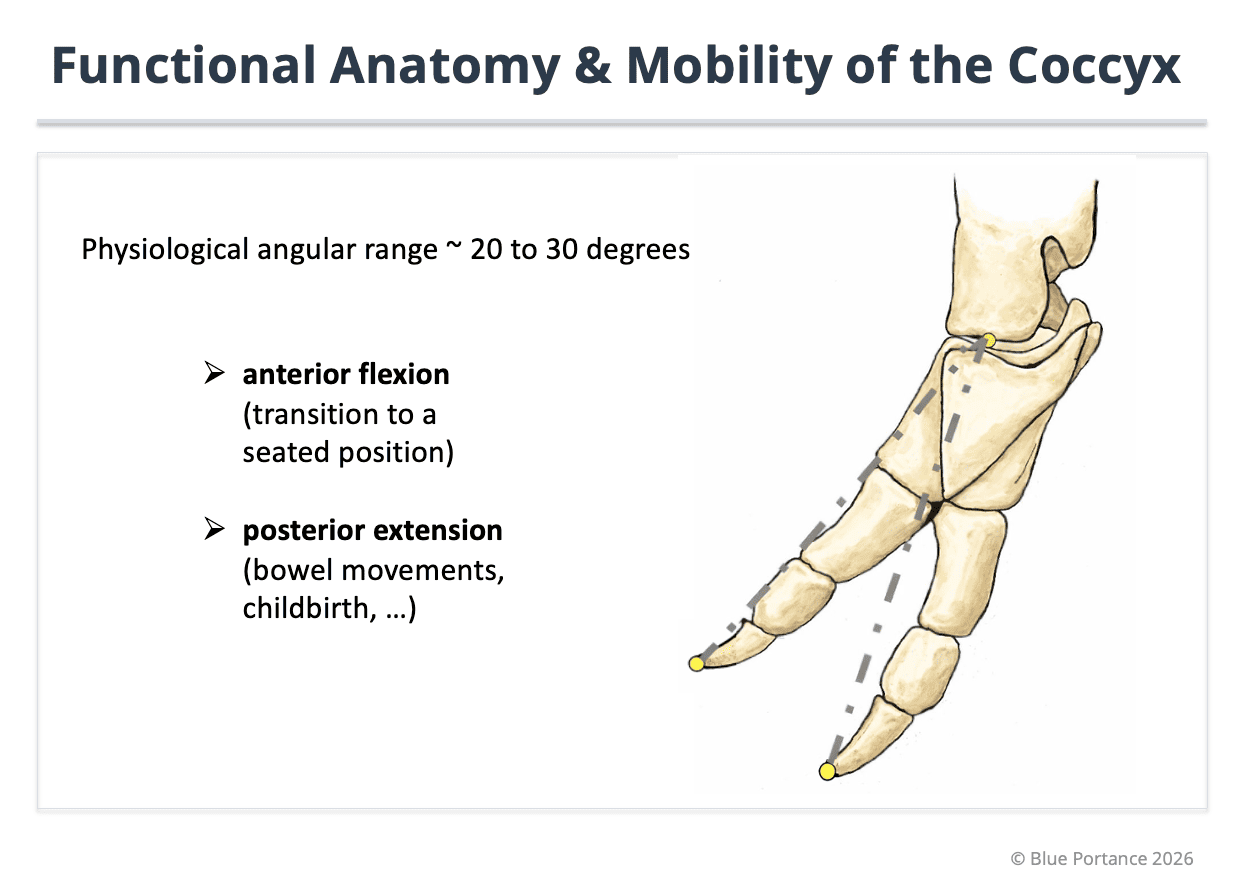
The coccyx can be compared to a small articulated lever: when it functions within its normal range, it protects the system; when it becomes mechanically dysfunctional, every posture change becomes more difficult.
You can explore this in more detail in our page on functional anatomy and biomechanics of the coccyx.
3. Mechanical Causes: What Actually Goes Wrong?
A. Falls, Impacts, and Forgotten Trauma
The most common cause of coccygodynia is direct trauma: a fall on the buttocks, a slip, a sports accident, or repeated shocks. The initial injury is often minimized—or simply forgotten—once the acute phase has passed.
Yet the coccyx may remain mechanically altered, sensitive, or less adaptable long afterward.
B. Childbirth: A Specific Mechanical Context
For some women, childbirth represents a major mechanical challenge for the coccyx. During delivery, the coccyx must move backward to increase the pelvic outlet. If this movement is excessive or constrained, it may leave lasting mechanical consequences.
C. Prolonged Sitting: The Silent Micro-Trauma
Not all coccyx pain starts with a fall. Long periods of sitting on hard or poorly adapted surfaces may repeatedly concentrate pressure on the ischial bones—and sometimes directly on the coccyx. Over time, these micro-constraints can contribute to persistent pain.
This is one reason why prolonged sitting can become a major mechanical stressor .
These mechanisms are part of a broader set of factors described in mechanical causes of coccydynia.
4. Local Pain or Referred Pain: When the Coccyx Blurs the Picture
In its typical form, coccygodynia presents as a strictly localized pain, worsened by sitting or by transitions between sitting and standing. In some cases, however, the pain becomes more diffuse and may spread toward the buttocks, lower pelvis, or perineal area.
This is where interpretation becomes difficult: the coccyx may still be involved, but the painful experience is no longer limited to one obvious anatomical point. Referred pain patterns may mask the true source of stress and make the mechanism harder to identify.
If you are trying to understand recurring tailbone pain when sitting, this distinction is essential.
To better understand how pain may spread or be misinterpreted, see local vs referred pain mechanisms.
5. The Coccyx at the Heart of the Pelvic Sling
The coccyx is never isolated. It forms the lower anchor point of a broader muscular and fascial system: the pelvic sling. This means that coccyx pain is not always about the bone alone.
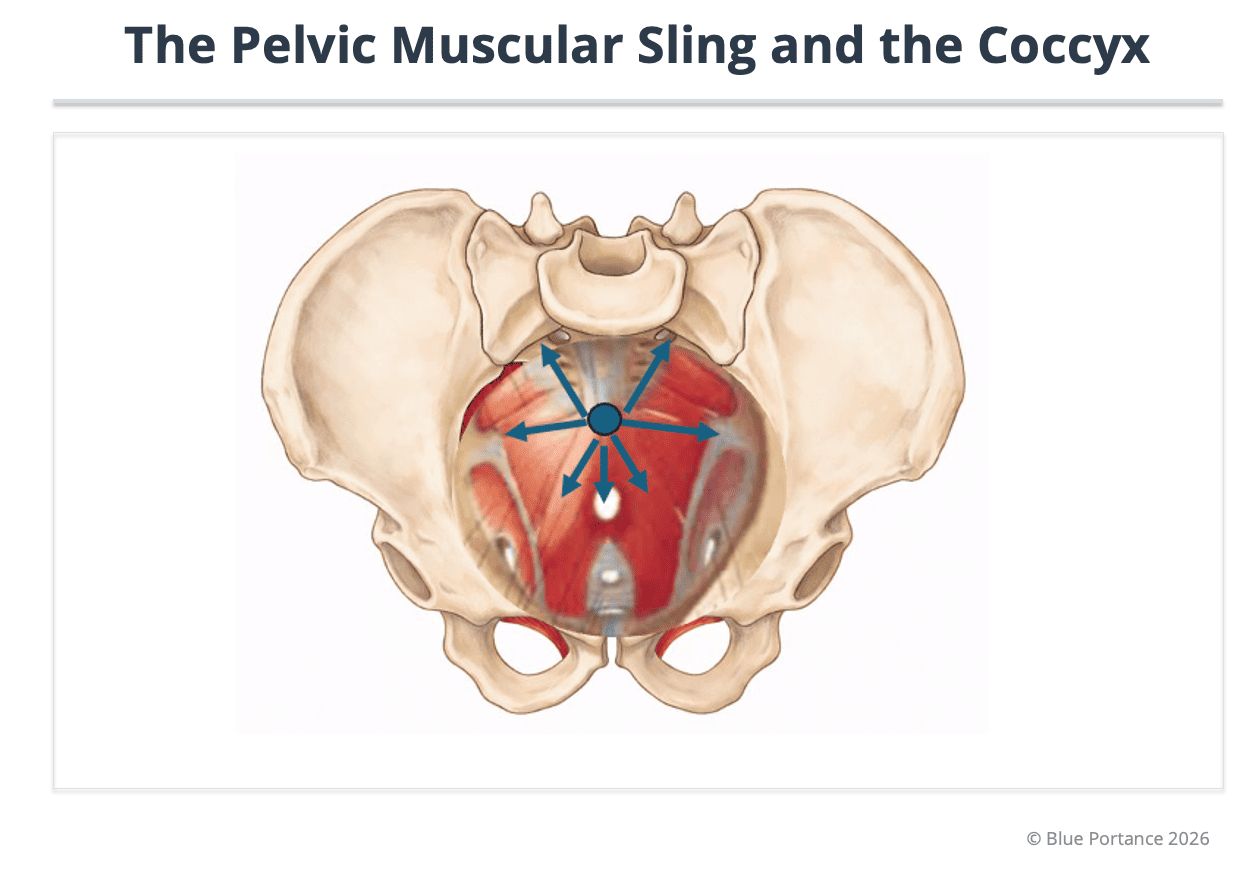
This is why some situations feel confusing: imaging may appear normal, yet the pain is very real, because the problem may remain functional long before any visible structural lesion appears.
Fascia plays a major role in this environment. You can explore this further in our fascia FAQ.
These interactions are also closely linked to nearby neural structures, further detailed in pudendal nerve anatomy.
6. Structural or Functional: The Question That Changes Everything
Some cases of coccygodynia are linked to identifiable structural changes: dislocation, excessive hypermobility, or a coccygeal spur. In such cases, the pain is associated with a more fixed mechanical alteration.
In many other cases, however, no obvious lesion is found. This is what may be called functional coccygodynia: the coccyx itself is intact, but it operates within a system that has lost its capacity to adapt.
Functional coccygodynia is not “pain without a cause.” It is pain without a visible lesion.
This distinction is central because it changes the logic of interpretation. The question is no longer only “what is damaged?” but also “what has lost its adaptability?”
This broader distinction is explored in our page on structural vs functional mechanisms .
Why Sitting Hurts So Much
Sitting is not a passive state. It is a mechanical situation in which the pelvis, spine, soft tissues, and support surface must continuously negotiate pressure and stability. When this negotiation fails, the coccyx may become the terminal point where unresolved constraints accumulate.
🔒 When the System Can No Longer Adapt
In a healthy system, loads are constantly redistributed through subtle movement and continuous micro-adjustments. But when mobility margins are reduced, when tissues stiffen, or when protective tension increases, pressure is no longer spread efficiently.
🟢 When Pain Becomes Progressive
This is why coccygodynia often becomes worse the longer one remains seated. Pain may not begin immediately. It can build gradually as the same tissues are loaded again and again without sufficient variation or release.
The result is not random pain, but the expression of a system that has lost part of its dynamic adaptability.
7. Summary: When Pain Becomes Understandable, It Stops Feeling Absurd
- The coccyx is a small but mechanically important structure.
- Its physiological mobility is limited, but essential.
- Trauma, childbirth, and prolonged sitting can all disturb load distribution.
- Coccyx pain may be local—or part of a broader referred or functional pattern.
- The key distinction is often structural versus functional, not “real” versus “imagined.”
The coccyx is not a secondary bone. It is a terminal point for load transmission. When it becomes painful, it is often because it is absorbing stress on behalf of a system that can no longer adapt smoothly.
Understanding that logic does not solve every case—but it changes the way the pain is interpreted. Once pain becomes understandable, it stops seeming absurd.
Your Experience
Your feedback, personal experiences, and constructive disagreements are welcome. The goal is to improve collective understanding of what happens mechanically when sitting becomes painful.



Kindly make the geal injection type to relief this bone kindly work on it
Thank you for your comment.
If you are referring to gel-based injections for tailbone pain, it is important to note that such procedures fall under medical treatments that must be evaluated and approved by regulatory authorities such as the U.S. Food and Drug Administration.
These injections should only be prescribed and administered by qualified healthcare professionals, based on an individual medical assessment.
This article does not provide medical advice and focuses on non-invasive, mechanical aspects of sitting-related coccyx pain.
For any injection-based treatment, we strongly recommend consulting a licensed medical professional.